Enteroclysis: The Small Bowel Enema (cont.)

Duodenal Intubation
(cont.)
|
- After the catheter tip is in the antrum, turn the
patient into a steep left posterior oblique (LPO) position. Push the
catheter distally. When the tip of the torque cable is at the level of the
duodenal bulb, fix the position of the tip of the cable, and advance the
catheter off of it into the duodenal loop. Do not push the torque cable
into the duodenal loop, as perforation of the gut wall might result.
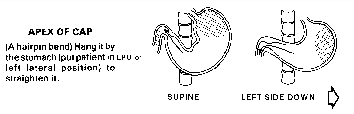
(Drawings modified from
pamphlet, "Duodenal Intubation, A 5-Minute Method",
Cook, Inc., Bloomington, IN,
copyright 1985)
- If, as sometimes happens, the catheter
coils in the fundus of the stomach, withdraw the catheter to the
gastroesophageal junction and again advance it as in steps 5 and 6. If
this fails, remove the torque cable and instill a small amount of barium
or air through the catheter to provide a visual marker of the
gastroduodenal anatomy.
- After the catheter tip has been advanced into the 4th
part of the duodenal loop, return the patient to the supine position. The
final placement of tip of the catheter should be in the region of the
ligament of Treitz, either in the distal duodenal loop or the proximal
jejunum.
- Tape the catheter to the patient's nose to prevent
migration of the tube.
-
If a balloon catheter is used, the balloon may be inflated with as
much as 15 ml of air to prevent duodeno-gastric reflux. The balloon should be inflated during fluoroscopic observation after infusion of a small volume of barium sulfate suspension into the small bowel (to prevent overdistention). Of course, if the
balloon is inflated, it must be deflated prior to removal of the catheter
at the end of the procedure.
|
|
|


![]()


