A pancreatic abscess is an
intra-abdominal collection of pus near the pancreas, and contains little
or no necrosis. Pancreatic abscess usually begin to form within 7-14 days after
an episode of acute pancreatitis, but they may present much later.
Approximately 2-6% of patients with acute pancreatitis develop a
pancreatic abscess. Abscesses may
be suspected in patients with spiking fever. In
suspected cases, US and CT are indicated for diagnosis and percutaneous
drainage. In cases of failed percutaneous drainage, surgical
intervention is indicated.
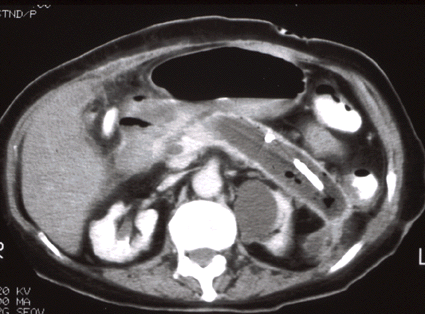
Radiologic findings of an abscess include a low density center, rim
of enhancement, and possible gas bubbles (more specific). The
table below compares US versus CT in the diagnosis of abscesses.
Diagnosis may be confirmed by radiographic-guided aspiration.
|
 |
|
Comparison of US versus CT in
Abscess Diagnosis |
| US |
CT |
-May be done at bedside
-Most effective in RUQ, peridiaphragmatic
-Gas may limit exam of mid abdomen
-Unable to definitely R/O abscess |
-Gives all encompassing image
-Not affected by bowel gas
-Clearly identifies bowel for access route planning |
Catheter
Management:
Following appropriate diagnosis, and radiologic and surgical
consultation, CT guided needle aspiration may be performed. In
cases of abscesses that yield pus, a catheter may be placed to drain the
purulent fluid. The cathater is placed on suction (connected to a
Jackson-Pratt bulb), and should be irrigated with saline each shift.
Patient's temperature, WBC, and drainage volume are monitored. A
decrease in temperature should be expected in 24-48 hours; the WBC count
should decrease within a week. The catheter may be pulled upon
resolution of symptoms, normalization of vitals/WBC, decrease of abscess
cavity size (as measured by repeat CT/US), and cessation of
drainage. Percutaneous drainage (PCD) is effective in 40% of
patients as the sole method of treatment. Studies have shown PCD
of abscesses to be more effective than surgical methods, with lower
mortality, complications, and recurrence.
|
![]()
![]()